APRIL 2015
|
The Surgical Technologist
|
163
the skin and pectoralis muscle into thin and undesirable tis-
sue. In most cases, the pectoralis provides little assistance in
daily living activities and will continue to atrophy following
the dissection.
Once released, the skin is then dissected from the mus-
cle following the pectoralis tendon high into the axilla to
create the anterior portion of the passageway needed for the
latissimus dorsi flap. Damp sponges are placed into the chest
wound and attention was turned to the patient’s back.
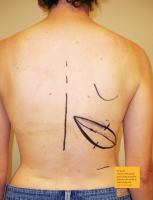
A 17 x 7 cm ellipse was previously marked obliquely on
the patient’s back following relaxed lines of tension. The
superior edge of the cutaneous flap outline is used for the
initial incision. This edge is injected with local containing
epinephrine, incised and the incision was carried down to
the latissimus muscle. The superior cutaneous flap is raised
first and dissected toward the axilla. The skin is temporarily
pulled inferiorly and manipulated to ensure that the donor
site as marked can be comfortably closed. The inferior bor-
der of the cutaneous flap is incised and taken inferiorly until
8 cm of latissimus muscle is exposed. The cutaneous paddle
is intentionally placed high on the latissimus muscle to allow
for the suturing of the muscle to the inframammary fold at
closure. The distal end is dissected away from its origin at
the posterior crest of the illium and is continued from the
lateral surface of the lumbar vertebrae (L1-5), thoracic ver-
tebrae (T7-12) and the posterior surface of the lower three
ribs.8 Larger perforating blood vessels are ligated and divid-
ed using hemoclips. The muscle harvest is then completed
and the pedicle remains attached. Precautions are taken to
not elevate the serratus muscle or any of its fatty tissues and
to protect the serratus branch of the thoracodorsal trunk.
If the blood supply from the main thoracodorsal trunk has
been sacrificed at the time of mastectomy, collateral circula-
tion via reverse flow from the serratus branch of the artery
can provide alternate blood supply.
Once a clear tunnel is formed via the axilla, a 2-0 nylon
suture is placed in the lateral edge of the musculocutaneous
flap to assist in transfer and correct orientation through the
axilla. The suture should pass through both skin and muscle
to prevent traction on perforating vessels while the flap is
passed through the tunnel. This flap is then passed to the
front of the patient and is stapled into place and covered
with an antimicrobial incise drape for a temporary hold dur-
ing repositioning.
Two 15-round Blake drains are placed inferior to the
wound edge using a #15 blade for the stab incision and sewn
into place using a 3-0 nylon suture. The wound is closed
with 3-0 and 4-0 polyglactin 910 at the deep and superficial
layers. A 4-0 poliglecaprone 25 is used to close the skin.
For the transition, the CST remains sterile as the sur-
geon and first assist remove the drapes and beanbag and
reposition the patient to the supine position for the tissue
expander placement and flap inset. Removal of the bean-
bag allows for the patient to be safely seated in the upright
position during the next phase of the procedure. The arms
are rested comfortably on ratcheted arm boards that have
been prepared using a 90-degree wedge covered with one
egg crate and a blue towel. This is secured to the arm board
using three bands of silk surgical tape. The arms are placed
in an abducted position to relax the pectoralis muscles dur-
ing surgery and minimize traction on the brachial plexus.
A second egg crate is placed over the patient’s arm, covering
from elbow to wrist and a gauze bandage roll is used to cir-
cumvent the padding. This is secured with two bands of silk
tape. Special attention is paid to the IV site, ensuring the IV
clamps and flanges do not press into the patient’s skin once
draped. If this is a concern, a 2x2 gauze can suffice as pad-
ding between the IV tubing and the patient. It is crucial the
arms and padding are tightly secured to the arm boards as
the patient will be placed in a sitting position intermittently
throughout the procedure. Finally, a pillow is placed under
the patient’s knees to relieve lower back strain and a safety
strap is placed two inches above the knee.
Once the patient is secured, she is placed in a full upright
sitting position by use of the mechanical bed. The surgeon
then adjusts the patient’s shoulders, arms, hips and torso
until the patient is sitting straight and shoulders are level.
The patient is returned to the supine position, the antimi-
crobial incise drape is removed and the patient’s skin is
again prepped from the chin to umbilicus and down to table
level. New drapes are placed and any equipment that may
have had its sterility compromised is replaced. The patient
is again draped and the surgeon and assistant change their
gown and gloves, before all staples are removed from the
flap site and the previously dissected pocket is checked for
hemostasis.
Attention is now turned to elevating the inferior mastec-
tomy flap appropriately. Prior to beginning the surgery, the
inframammary fold was marked bilaterally on the patient.
Dissection to the inframammary fold is done carefully, and
symmetry is checked against the opposite side by bringing
the patient to an upright position. If uncertain, the fold also
can be checked against the approximate site of the pectorals
muscle insertion. The subpectoral dissection is performed
by transecting the pectoralis muscle from the inframam-