|
The Surgical Technologist
|
APRIL 2015
164
mary fold and leaving a small cuff at the medial insertion
site. The edge of the latissimus muscle is sewn into the
medial cuff of the pectoralis muscle at the inframammary
fold using 3-0 polyglactin 910s in an interrupted figure-
eight fashion.
The width of the pocket is then measured and a compat-
ible expander is chosen. The pocket is copiously irrigated
with triple antibiotic irrigation and wound edges painted
with betadine solution. The triple antibiotic irrigation is
comprised of 100,000 units of bacitracin, 160mg of cefazolin
and 2 grams of gentamicin mixed with a liter of 0.9% saline.
The surgeon changes its gloves and the expander is opened
to the back table and bathed in triple antibiotic solution.
The tissue expander is infolded so as to
present the back plate at the inframa-
mmary fold and completely flattened
prior to insertion by using suction and
a 21-gauge butterfly needle placed into
the central port causing the air to be
completely evacuated. If the expander
is tabbed, the tabs are sewn in with 3-0
polyglactin 910 sutures. These tabs are
located at the 4, 6 and 8 o’clock orien-
tation of the expander. This technique is used to maintain
positioning during post-op fill and the 3 to 6 months the
tissue expander will remain implanted to allow the skin
and muscle to relax and expand. Sterile injectable saline
is added to the expander via the same 21-gauge butterfly
needle found within the manufacturer’s packaging of the
expander. The expander is filled just enough as not to cause
undue stress and tension on the skin. After being filled, the
amount of saline is documented in the patient’s chart along
with the style, size and manufacturer’s tracking number of
the implant. A dose of 10 mL of 0.5% bupivacaine hydro-
chloride is placed into the pocket via a 10 mL control-top
syringe without a needle attached. The remainder of the
latissimus muscle is inset into the fold and laid out along
the lateral edge of the tissue expander to provide full muscle
coverage of the tissue expander. Superiorly, the latissimus
muscle is draped over the pectoralis muscle and 3-0 poly-
glactin 910s are used in a figure-eight fashion to tack the
edge of the latissimus to the pectoralis. A third 15-round
Blake drain is placed through a stab wound and the drain is
placed into the lower aspect of the pocket. The drain is sewn
in with a 3-0 nylon suture.
If necessary for adequate and aesthetically pleasing clo-
sure, the mastectomy flap is tailored. If the patient has been
radiated, this tissue is often very thin and does not stretch
well. The tissue from the tailoring is then set to pathology
as mastectomy scar and reviewed for any cancerous signs.
The musculocutaneous flap is also tailored and inset with
3-0 and 4-0 polyglactin 910s and a 4-0 poliglecaprone 25 is
used at the skin.
Once all sutures and bulbs for the drains are placed, the
drapes are removed and the remaining blood and fluids
are wiped from the patient. A binder is placed to secure
all dressings and provide slight compression on the wound
sites. The circulator properly labels all drains to identify
side, date, location and size of drain. The drains are secured
to the patient’s binder and the Foley catheter is left in place.
The patient is reversed, extubated and taken to the
recovery room. All sponges and needles counts are counted
prior to closure.
S P E C I A L C O N S I D E R A T I O N S
The skin of the back is slightly different in both color and
texture than the skin of the chest. Many patients will have
varying levels of skin differences of their reconstructed
breasts. The reconstructed breasts will also have little to no
sensation. The reconstructed nipples have no sensation at
all as they are constructed from the skin and fatty tissues of
the transferred skin. The areola color for the nipple recon-
struction can be tattooed on with medical grade ink during
an office visit. Patients are encouraged to match the color of
their areolas to a color sample prior to mastectomy.
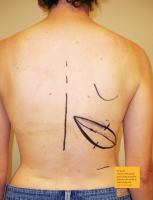
Patients will have one or two scars on their back that
may prove to be difficult to hide under a bra or swimsuit.
These scars can be horizontal, slightly diagonal or longitu-
dinal along the lateral aspect of the body depending on the
surgeon’s approach.
If the inframammary fold is compromised during the
mastectomy, or the patient has elected an immediate recon-
struction, the surgeon may opt to use a cadaver derived
implant or an animal-derived implant called. These dermal
grafts are used within the wound and sewn to the fold using
non-absorbable braided sutures in a figure-eight pattern.
Once the patient is properly positioned and
draped, the first incision is performed on the
chest, through the previousmastectomy scar.